
WHITE PAPER: A Fresh Look at Professional Liability in Orthopedics Given Recent Extraordinary Judgments in Sports Medicine
Theodore Schlegel, MD, President and Chief Medical Officer, AOP
David Berman, Senior Data Consultant, AOP
Lee Newmark, Area Executive Vice President, Gallagher
June 2024
Key Takeaway
Recent legal precedents have significantly changed the landscape of the malpractice insurance industry for America’s orthopedic surgeons. All professional liability insurance (PLI) companies are absorbing the impact of new liabilities, which are certain to lead to significant rate hikes going forward.
This is forcing all buyers to rethink their strategy for how they obtain PLI coverage. What worked for the past decade will simply not produce the results that are desired by physicians and their executive teams.
Severe awards (of over $10 million) are beginning to undermine the pricing and availability of professional liability insurance. Given recent enormous judgments awarded to professional athletes, now is a good time to review the fundamentals of professional liability insurance (PLI) for community orthopedic practices.
What’s driving the increase? As salaries have risen for professional athletes, and as college and even some high school athletes have secured lucrative Name Image Likeness (NIL) deals, the liability for future earnings has increased markedly. If your practice takes care of athletes at any level, including high school, you should be aware of the potential for extraordinary malpractice risk.
While collegiate and professional team physicians are expected to be credentialed in sports medicine, no such requirements are in place for most high school team physicians. The civic-minded community physicians who provide high school team coverage often are orthopedists who may not yet understand the new high liability inherent in NIL.
NIL ushers in a new level of risk, but issues regarding the cost and availability of PLI for surgeons have been festering for years. It’s instructive to look at Canada to see what might happen. Twenty-one years ago, in 2003, almost all Canadian physicians who treated professional athletes lost their malpractice coverage at once when the Canadian Medical Protective Association, a mutual insurance cooperative that insured 95 percent of the doctors in Canada, stopped offering coverage. The Association decided that the financial risk of insuring physicians who care for professional athletes was too high. Note that this was a decision made by physicians to protect the affordability of the entire system. The cost of the malpractice coverage was shifted to the teams.
Social inflation is also putting substantial upward pressure on the cost of PLI. Between 2014 and 2020, U.S. inflation rose roughly 15 percent while the cost to resolve the average paid medical malpractice claim rose by 42 percent. Social inflation is doled out one verdict and one settlement at a time…very large verdicts exert upward pressure not only on the size of other verdicts but also on targets within settlement negotiations.[1]
Professional Liability and Orthopedic Surgery
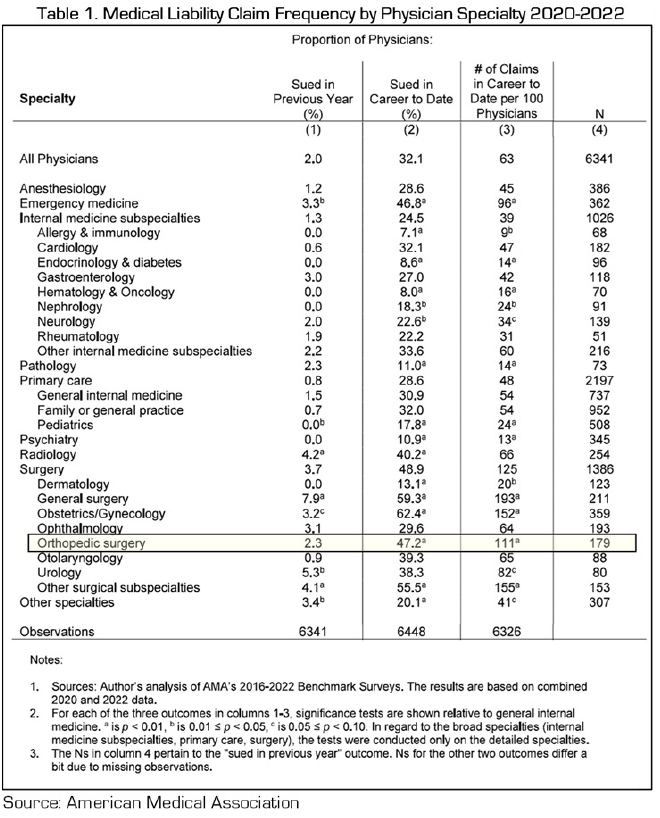
Compared to other specialties, orthopedic surgeons are sued a lot, but not the most. Table 1, from the American Medical Association, presents claim frequency by specialty over the previous year, career to date, and number of claims career to date per 100 physicians. During their careers, 47.2 percent of orthopedists have been sued at least once. This is the 4th highest rate of all specialties, behind OB/GYN (62.4 percent), general surgery (59.3 percent), and other surgical subspecialties (mostly neurosurgery; 55.5 percent). The same is true in terms of number of claims over a career per 100 physicians; orthopedic surgery is 4th at 111 claims (or 1.11 claims per physician), behind the same 3 other specialties.
Orthopedists also don’t have the highest malpractice premiums, but we do pay significantly more than most other specialties.[2] OB/GYNs pay the most. Then come neurosurgeons. After neurosurgery, premium rates are high and similar for orthopedics, thoracic, plastic, general surgery, ophthalmic surgery, emergency medicine, and gynecology.[3]
It may seem obvious, but orthopedic surgeons pay high malpractice premiums because orthopedic surgeons do high volumes of surgeries and procedures. The total number of orthopedic surgeries/procedures performed in the US was estimated to be 18,575,000 in 2022.[4] [In comparison, OB/GYNs deliver about 3.6 million babies annually.] Over 1 million of the orthopedic procedures are total hip and knee replacements, the demand for which continues to grow rapidly. The total also includes orthopedic bone cement and casting material procedures, orthobiologic procedures, arthroscopy procedures, spinal surgery procedures, knee reconstruction procedures, trauma fixation procedures, shoulder replacements, and other joint reconstruction procedures. We are normally very busy physicians.
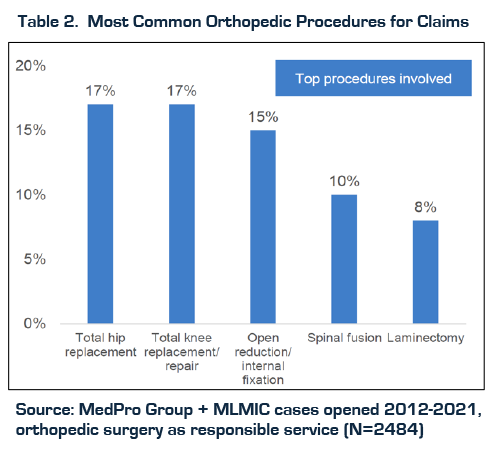
There are a few lessons we can learn from analyzing malpractice claims. MedPro, a large provider of PLI, looked at 2,484 orthopedic procedure malpractice claims opened between 2012 and 2021 and found that the 5 most common procedures involved are total hips, total knees, open reductions, spinal fusion and laminectomy. Together, these account for about two-thirds of the total. [Table 2]
The Doctors Company, another large provider of PLI, looked at 453 hip and knee replacement closed claims between 2009 and 2019 and found:
- The top three major intraoperative injuries were related to an aggravated or worsened preoperative condition, like pain or mobility (19 percent), nerve damage (16 percent), and/or postoperative pain (13 percent).
- Infections, including nosocomial infections, are more common in the ambulatory setting. One explanation may be lower compliance with the antibiotic dosing regimen, as the third and final dose relies on the patient at home.[5]
- Cases are often related to a surgeon’s delayed or inadequate response to developing complications.
Extraordinary Judgments in Sports Medicine
The safety and well-being of athletes is the top priority of sports medicine physicians and their teams, who are responsible for providing care to keep athletes in the game and enjoying what they love. But mistakes at the professional level can be very costly.
- Former Minnesota Vikings defensive tackle Sharrif Floyd filed a $180 million medical malpractice lawsuit against famed orthopedic surgeon Dr. James Andrews[6] and ten other defendants. Floyd charges that he suffered debilitating muscle and nerve damage in the aftermath of an unpermitted knee surgery at the Andrews Institute in Pensacola in September 2016. Subsequently, Floyd and Andrews reached a settlement for an undisclosed amount. Floyd is now suing four malpractice insurers and brokers for breach of contract, alleging that only $17 million was paid out of $27 million in coverage available.[7]
- In 2023, former Eagles safety Chris Maragos was awarded $43.5 million in a medical malpractice lawsuit in connection with his career-ending knee injury. A jury found Dr. James Bradley and Rothman Orthopaedics negligent and ordered the surgeon to pay about $29.2 million and Rothman around $14.3 million. Maragos contended in court that the case cost him at least $8.7 million in future NFL earnings but was awarded five times that in total.
- Former New York Giants running back Michael Cox won $28.5 million in September 2022 in a lawsuit over a failed ankle surgery that ended his career.
- Former L.A. Chargers quarterback Tyrod Taylor is suing Chargers’ team doctor David Gazzaniga for at least $5 million after a quick pre-game injection meant to manage rib pain resulted in a punctured lung.
Our industry continues to push back. In June of 2023, the American Orthopaedic Society for Sports Medicine (AOSSM), along with 27 co-signers, distributed an open letter saying that “recent and ongoing litigation may have an enormous negative impact on the medical care of competitive and elite athletes.” AOSSM’s primary concern is that the nation’s top doctors and surgeons may refuse to care for high-level athletes of all ages. Additionally, AOSSM wants a higher standard for expert testimony in malpractice cases involving athletes.
In a 2023 interview with ESPN, Dr. Mark Miller, AOSSM’s President, explained the society’s reasoning:
“If not now, when? We want to raise public awareness that this issue affects the care of all people we take care of. Our ability to serve all of our patients from the playground to the professional level is at risk.”
Dr. Scott Rodeo, the head team physician for the New York Giants, expressed similar views to ESPN:
“Recent cases may be the tip of the iceberg, and some physicians may decide the visibility associated with caring for athletes may not be worth the liability risk anymore.”
In partnership with Gallagher, a national leader in providing medical professional liability solutions to the physician community, AOP is creating an innovative program for favorable professional liability coverage to our physician partners. We could be doing the same for you.
For more information, please contact Ted Schlegel at [email protected] or Lee Newmark at [email protected].
Footnotes:
[1] Paraphrased from Robert E. White, Jr, The Doctors Company. See references.
[2] Orthopedic Surgery is broken into 3 classifications by medical malpractice insurance carriers: Surgery No Spine, Surgery with Spine, or No Surgery. Spine surgery coverage costs the most; no surgery the least.
[3] eQuoteMD.
[4] United States (US) Orthopedic Procedures Count by Segments and Forecast to 2030. See references.
[5] The Doctors Company, Hip and Knee Replacements article, page 5. See references.
[6] Disclosure: Dr. Andrews is a former Board member of AOP.
[7] Business Insurance reported Jan. 20, 2023.
References:
Protecting Athletes and Team Physicians Who Care for Them Amid Rising Complexity and Liability Risk, American Orthopaedic Society for Sports Medicine (AOSSM), Open Letter, June 12, 2023
https://www.sportsmed.org/about-us/news/protecting-athletes-and-team-physicians-who-care-for-them-amid-rising-complexity-and-liability-risk
A Deep Dive Into Sharrif Floyd’s $180 Million Lawsuit Against Dr. James Andrews, Sports Illustrated, Michael McCann, November 6, 2018
www.si.com/nfl/2018/11/07/minnesota-vikings-sharrif-floyds-180-million-lawsuit-against-dr-james-andrews
Former Eagles captain Chris Maragos awarded $43.5 million in lawsuit over career-ending injury, The Athletic Staff, February 13, 2023
https://theathletic.com/4192466/2023/02/13/chris-maragos-lawsuit-knee-injury/
Hip and Knee Replacements: An Examination of Malpractice Claims Against Orthopedic Surgeons From the Ambulatory and Inpatient Settings, Jacqueline Ross, RN, PhD, Coding Director, Department of Patient Safety and Risk Management, The Doctors Company, August, 2022
https://www.thedoctors.com/contentassets/63dbc3e1dd414ef29cf6cff67847df8b/hip-and-knee-replacements-closed-claims-study_082522.pdf
Med mal concerns sideline physicians for sports teams, Business Insurance, April 20, 2003
https://www.businessinsurance.com/article/20030420/STORY/100012697?template=printart
Medical groups: Liability may limit care for top athletes, Stephania Bell, ESPN, June 12, 2023
https://www.espn.com/espn/story/_/id/37841581/medical-groups-alarmed-rising-liability-costs
Medical Liability Claim Frequency Among U.S. Physicians, Jose R. Guardado, PhD, American Medical Association, May 10, 2023
https://www.ama-assn.org/system/files/policy-research-perspective-medical-liability-claim-frequency.pdf
Medical Malpractice and the Volunteer Team Physician, Michael C. Koester, MD, Slocum Center for Orthopedic and Sports Medicine, The Doctors Advocate, Fourth Quarter, 2023
https://www.thedoctors.com/the-doctors-advocate/fourth-quarter-2023/medical-malpractice-and-the-volunteer-team-physician/
MedPro Professional Liability Data, Orthopedic Surgery, Claims Data Snapshot, MLMIC Insurance Company, 2023
https://www.medpro.com/documents/10502/5086243/Orthopedics.pdf
Risking Life for Limelight: Medical Malpractice in the NFL, Christopher T. Nace, The Legal Examiner, February 9, 2023
https://washingtondc.legalexaminer.com/health/risking-life-for-limelight-medical-malpractice-in-the-nfl/
Who Pays the Highest Rates for Medical Malpractice Insurance? eQuoteMD
https://www.equotemd.com/2022/10/07/who-pays-the-highest-rates-for-medical-malpractice-insurance/#:~:text=So%2C
United States (US) Orthopedic Procedures Count by Segments and Forecast to 2030, Global Data, February 17, 2023
https://www.globaldata.com/store/report/usa-orthopedic-procedures-analysis/#:~:text=US%20Orthopedic%20Market%20Report%20Overview,on%20the%20US%20Orthopedic%20Procedures.
Social inflation drives up malpractice payouts—and insurance rates, Medical Economics, Robert E. White, Jr., May 18, 2023
https://www.medicaleconomics.com/view/social-inflation-drives-up-malpractice-payouts-and-insurance-rates












Sorry, the comment form is closed at this time.